Beyond-Truth
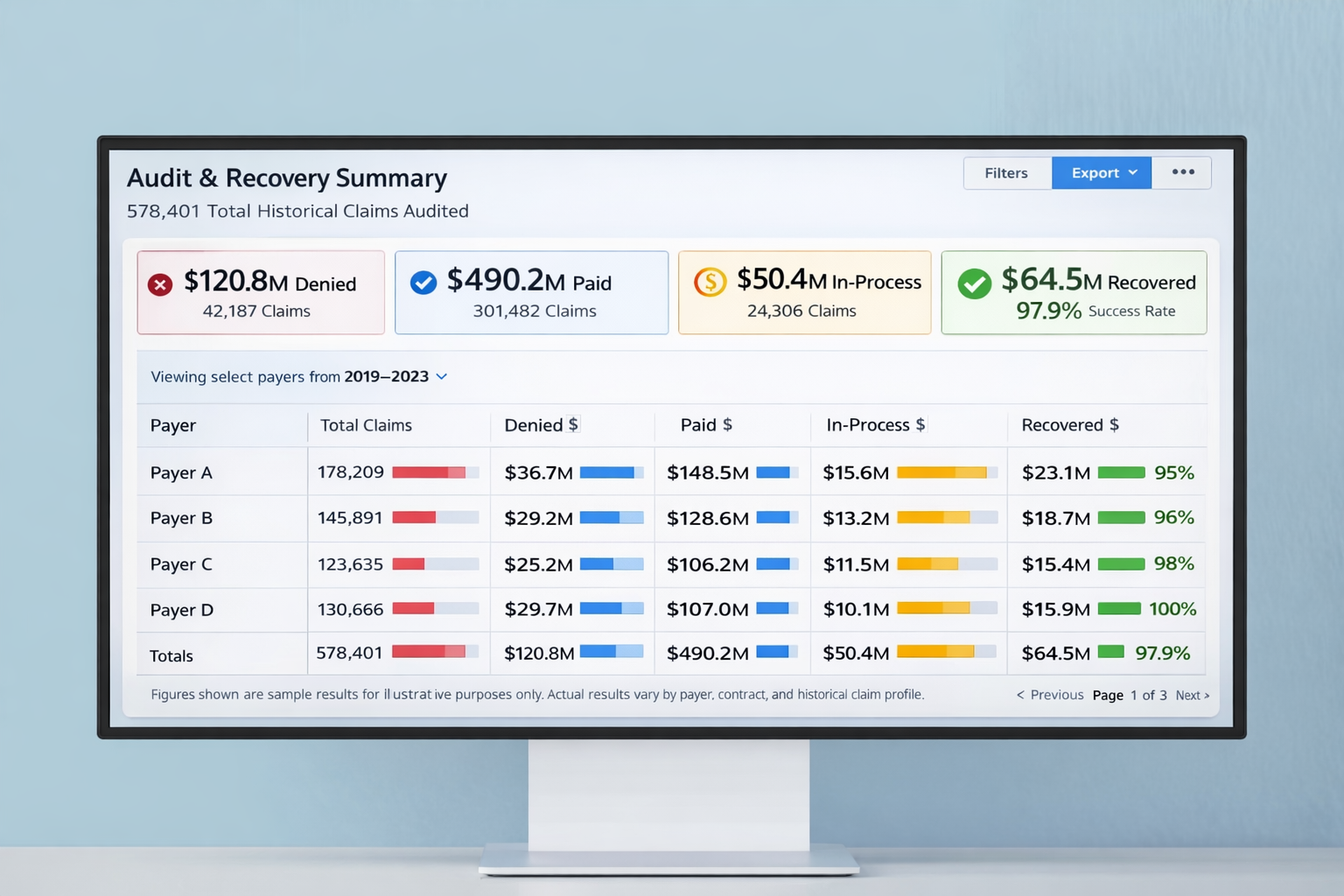
Beyond-Truth is the deterministic financial intelligence and recovery engine of the platform — built to identify what was underpaid, denied, missed, or written off too early, and to make those dollars visible, auditable, and actionable.
It answers the question leadership should have been able to answer years ago:
What revenue was truly earned, what happened to it, and what can still be recovered?
What Beyond-Truth Is
Beyond-Truth is not generic reporting and not black-box AI. It is a deterministic, auditable financial truth layer that evaluates claims and remittance history at service-line precision.
It is designed to expose denials, underpayments, partial payments, and transaction-level leakage that standard reporting often misses or treats as uneconomical to pursue.
What Beyond-Truth Does
- Audits paid and denied claims at the service-line level
- Identifies underpayments, denials, and financial leakage
- Distinguishes true recoverable dollars from noise
- Supports corrected claim generation and appeal workflows
- Makes smaller claims economically viable to pursue
- Provides leadership with auditable, explainable outcomes
What It Exposes
- Silent underpayments hidden inside paid claims
- Service-line discrepancies masked by aggregate posting
- Payer-specific enforcement inconsistencies
- Modifier, bundling, and adjudication-related leakage
- Claims written off because labor economics failed
- Recovery opportunity that traditional workflows never reached
These findings are grounded in actual transaction outcomes and deterministic evaluation logic, not estimates or optimistic guesses.
Why It Matters
Most healthcare organizations know denials matter, but they still lack a clean way to see the broader truth across denied, partially paid, and silently underpaid claims. That leaves leadership making decisions without a complete picture of what was really lost.
Beyond-Truth replaces conjecture with auditable financial reality, so recovery strategy can be based on evidence, not assumptions.
What Leaders Receive
- Quantified recovery opportunity by payer and service line
- Visibility into denied, underpaid, and partially paid claims
- Corrected claim and appeal workflow support
- Audit-ready documentation suitable for governance review
- Executive-level transparency into financial leakage
- A factual basis for recovery prioritization and action